Strengthen tobacco control to prevent 26 million cases of tooth loss
By Ziqi Chen, Gagandeep Kaur, Nadia Kaunein, Claireta Handoko, Marco A. Peres, Melissa Russell, Ankur Singh • Apr 6, 2026 • public health
Why This Matters
Tooth loss is often seen as an inevitable part of ageing; however, it is largely preventable. It may reflect years of advanced oral diseases, as well as a lack of timely treatment. Globally, the burden of tooth loss is huge. The 2021 Global Burden of Disease Study (GBD) estimated that 353 million people worldwide are living with edentulism (complete tooth loss). The consequences of tooth loss extend well beyond the mouth. People with tooth loss may struggle with limited eating and chewing ability, lack of confidence in social interactions, and face financial burden due to the high cost of dental work. Tobacco smoking, one of the biggest public health challenges in the world, does not spare the mouth. Tobacco use is also socially patterned, with higher rates among disadvantaged groups, contributing to health inequalities. But less is known about how tobacco use drives inequalities in tooth loss. We investigated whether tobacco smoking increased the risk of tooth loss, if more packs and years of smoking cause more tooth loss, and whether the effect is different between people from different socioeconomic groups.
What Was Done
We pooled data from all existing studies on smoking and tooth loss. Specifically, we examined whether current smokers and former smokers had a high risk of tooth loss compared to people who have never smoked. We also examined the effect of different smoking frequencies and intensities on tooth loss; including number of cigarettes per day among current smokers, and lifetime exposure to smoking among past smokers, both compared to never or non-smokers. In total, 30 studies were included in the systematic review, many of which were not included in previous systematic reviews or meta-analyses. We used robust assessment tools (like ROBINS E) and provided an updated picture of how smoking contributes to tooth loss as well as the effects of the intensity and lifetime exposure of smoking on tooth loss.
Key Findings
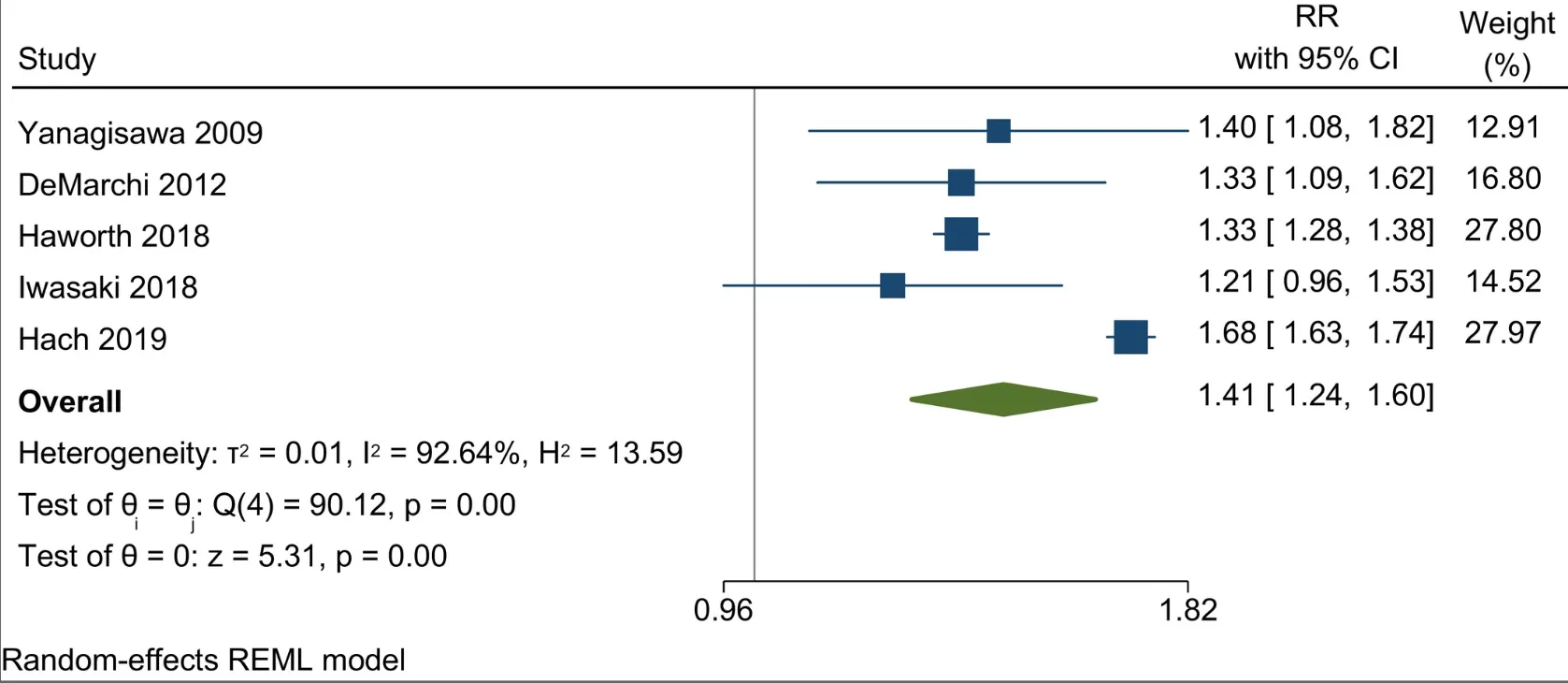
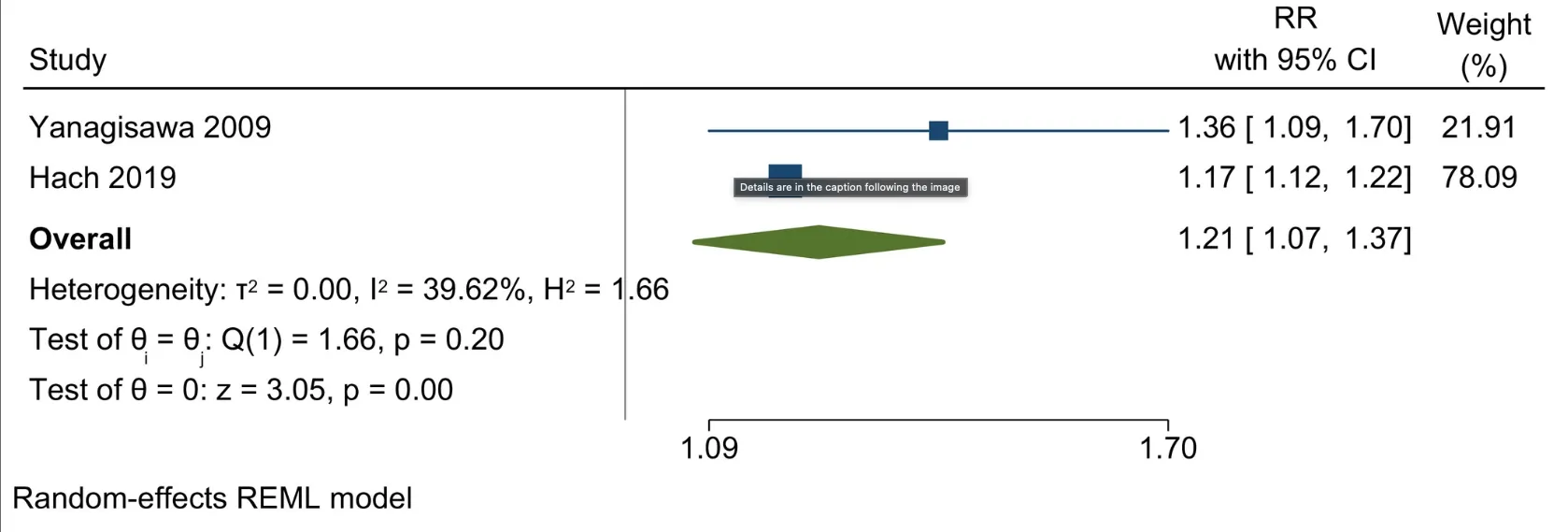
- Current smokers had a 40% higher risk of tooth loss compared to non-smokers.
- Past smokers had a 20% higher risk of tooth loss compared to never smokers, but lower than current smokers.
- Any level of smoking was harmful. Among current smokers, both heavy smokers and light smokers had a higher risk of tooth loss compared to non-smokers.
- If cigarette smoking were to be eradicated, around 1 in 14 cases of severe tooth loss, about 26.17 million cases globally, could be prevented.
- Most studies in this review were from high-income countries, with limited evidence from low- and middle-income countries.
What This Means for Equity & Policy
This study found strong evidence that smoking is a major driver of tooth loss. The lower risk among past smokers than current smokers highlights that quitting smoking can lower the risk of tooth loss.
Our findings also point to some important gaps in evidence. There have been few cohort or case–control studies on this topic from low- and middle-income countries, despite around 80% of current smokers residing there. Additionally, smoking-related oral diseases exhibit social inequalities that are more prevalent in these countries. Therefore, high-quality longitudinal evidence from low- and middle-income countries is needed to better understand the effects of tobacco smoking on tooth loss and inform public health policies and interventions in these regions. Additionally, smoking is known to be socially patterned, with higher rates among disadvantaged populations. Yet, none of the included studies examined how the effect of smoking on tooth loss differs across socio-economic groups. Future investigation is recommended to focus on social inequalities between smoking and tooth loss.
From a policy perspective, the findings of this study challenge current policies that neglect smoking cessation as part of standard oral care. Preventive strategies need to be developed and implemented to help individuals quit smoking for better oral health in clinical settings. This includes ensuring that oral health services are appropriately equipped to guide patients about smoking cessation for better oral health. It is also important to provide access to regular preventative care and promoting oral hygiene through government and community level initiatives.
Smoking cessation must be a key priority in oral health preventive strategies to prevent severe tooth loss and address social inequities in oral health outcomes.
Citation & Links: Ziqi Chen, Gagandeep Kaur, Nadia Kaunein, Claireta Handoko, Marco A. Peres, Melissa Russell, Ankur Singh. ‘The Effect of Tobacco Smoking on Tooth Loss: A Systematic Review and Meta-Analysis’, Journal of Clinical Periodontology. https://doi.org/10.1111/jcpe.70110